Removal of polyps without curettage of the uterus
A minimally invasive procedure aimed at removing polyps from the uterine cavity without damaging its structure. The method allows you to preserve a woman's reproductive function and increase the chances of a successful pregnancy.

Endometrial polyps are benign growths in the form of a rounded outgrowth on a thin leg that are attached to the mucous membrane of the uterus. They can cause profuse and irregular menstruation, bleeding between cycles, and abdominal pain.
Removal of polyps is important to prevent their growth and possible transformation into malignant tumors. Modern treatment methods allow not only to remove polyps without damaging the surrounding tissues, but also to perform a biopsy to exclude or confirm the presence of atypical cells. The operation is performed without curettage of the uterus, by hysteroscopy, which avoids damage to healthy tissues and the risk of adhesions in the uterine cavity. Careful surgical intervention promotes faster recovery, reduces the risk of complications and preserves a woman's reproductive function.
Before removing polyps, it is necessary to: Consult with a gynecologist Perform general blood and urine tests Perform an ultrasound examination (ultrasound) of the pelvic organs In some cases, hysteroscopy may be required.
Polyps are removed under visual control using a hysteroresectoscope equipped with a video camera. During the procedure, the doctor grabs the leg of the polyp and gently excises it, completely removing the polyp without damaging the surrounding healthy endometrial tissues. After excision, the polyp is aspirated (sucked out) from the uterine cavity. In addition, current cauterization (ablation) or laser techniques can be used to remove polyps, which help destroy the remaining cells of the polyp, reducing the risk of recurrence. All actions are performed inside the uterine cavity under visual control, the operation is practically bloodless and does not require incisions. The whole process takes about 20-30 minutes, and the patient can be discharged from the clinic on the same day.
To remove polyps, the following methods are used: Hysteroscope with video camera Surgical instruments (forceps, resectoscopes)
After removing the polyps, it is important to follow the doctor's recommendations. Spotting and mild discomfort are possible in the first few days after surgery. During this period, it is recommended to avoid physical exertion and not lift weights more than 5 kg, you should refrain from sexual activity, do not visit the sauna and steam room, and avoid hypothermia, especially pelvic organs, for 1-2 months after the procedure.
Benefits
Minimal injury
Reducing the risk of complications and accelerating recovery.
A short period of rehabilitation
Most women can return to normal life the very next day after the procedure.
High efficiency
The procedure allows you to completely get rid of polyps, preventing their reappearance.
Preservation of reproductive health
The removal of polyps does not affect a woman's fertility, allowing her to plan a pregnancy in the future.
Consultation before removal of polyps without curettage of the uterus
During the consultation, the gynecologist examines the patient, and diagnostics is performed, including ultrasound of the pelvic organs and, if necessary, hysteroscopy. This allows you to accurately determine the number, size and location of polyps.

The procedure for removing polyps without curettage of the uterus
The procedure is usually performed under short general anesthesia. A specialist inserts a hysteroscope through the cervix, a thin instrument with a camera. Single polyps on the pedicle are removed with scissors or forceps, which are inserted through the surgical channel of the hysteroscope. All manipulations are visualized on the screen, which allows you to perform the procedure accurately and efficiently.

Recommendations after removal of polyps without curettage of the uterus
After the procedure, it is important to follow the doctor's recommendations, including limiting physical activity and sexual activity for a short period of time. Medications may also be prescribed for the healing and prevention of infections.

Frequently Asked Questions
How often do I need to be checked for endometrial polyps?
Is it possible to get pregnant after removing polyps?
What sensations are possible after the procedure?
Are there any risks of recurrence of polyps?
Didn't find an answer to your question?
You can describe your problem in detail and ask a question to the doctor. He will answer you and help you find a solution
Врачи
Смотреть всех врачейCandidate of Medical Sciences. Gynecologist-obstetrician. Head of the gynecology department.
Obstetrician-gynecologist, specialist in operative gynecology, ultrasound diagnostician.
Doctor of the highest category, surgical obstetrician-gynaecologist specialising in anti-age and bioregenerative medicine, oncologist
Indications and contraindications
Indications
Detection of polyps in the uterine cavity
Polyps are often the cause of menstrual irregularities and bleeding.
Bleeding of unclear etiology
Irregular, profuse or intermenstrual bleeding that is not associated with other diseases of the reproductive system.
Menstrual disorders
Changes in the duration, regularity and intensity of menstrual bleeding.
Alleged infertility
Cases where polyps can cause difficulties with conception or unsuccessful IVF attempts.
Expected effect
Exclusion of bleeding
Normalization of the menstrual cycle, prevention of unpredictable bleeding.
Fertility recovery
Improving the conditions for conception.
Reducing the risk of developing cancer
Polyps can degenerate into malignant formations, their removal reduces the risk of developing endometrial cancer.
Improvement of general well-being
Improving a woman's quality of life.
Similar referral activities
Consultation of a gynecologist
Medical examination aimed at diagnosing, treating and preventing diseases of the female reproductive system.
Removal of tumors in the intimate area
A procedure aimed at eliminating benign growths such as papillomas, warts, cysts and genital warts.
Reproductive surgery
Surgical treatment and simultaneous accurate diagnosis of female infertility factors: adhesions, endometriosis, congenital malformations of the genital organs, obstruction of the fallopian tubes, intrauterine pathology (septum and synechia), polycystic ovary syndrome.
Cervical plastic surgery
Cervical plastic surgery (tracheloplasty) is a surgical restoration of the anatomical structure and function of the cervix, which helps to maintain the health of the reproductive system.
Treatment of vulvar diseases
Vulvar diseases, including chronic fissures, sclerotrophic lichen and other dermatological conditions. We offer modern and effective treatment methods aimed at reducing symptoms and restoring the normal condition of the vulva skin.
Correction of menopause problems
The onset of menopause is often accompanied by a number of physical and mental manifestations unpleasant for a woman. The gynecologist will choose therapy, which can relieve or completely eliminate the symptoms.
News & Media
All news and mediaThe III All-Russian Progress Conference "Aesthetic Gynecology and Perineology: balance of beauty and functionality" was held in Moscow
The event lasted from 24 to 26 May, and the theme was Aesthetic gynecology and perineology: the balance of beauty and functionality.
What to do with urinary incontinence after childbirth?
Find answers to your questions and feel more confident.
What is important for every woman to know about the cervix?
Everything you need to know about the cervix is now collected in one article on the website of the "Daughter-mother".
Why should your mother visit a gynecologist?
We all understand why girls should visit a gynecologist. This specialist will help solve various problems related to women's health — from pregnancy management to the prevention of sexually transmitted diseases. However, over time, when women get out of reproductive age, they begin to contact a gynecologist less and less often, mistakenly believing that they no longer need his help. But a gynecologist is not only about reproductive health, he can help in solving many other issues related to the female body. So what questions can your mother ask a gynecologist about?
How to strengthen the pelvic floor muscles?
Intimate problems are often hushed up, it is awkward to talk about them even with a doctor. However, if the issue concerns the health of the pelvic floor, it is better not to waste time and immediately consult a doctor. After all, problems with this area can lead to very unpleasant consequences.
Uterine bleeding — is it worth sounding the alarm?
Abnormal uterine bleeding is when the bleeding goes beyond the normal menstrual cycle. The discharge may be more abundant or last longer. The "normal" menstrual cycle is different for everyone. But menstruation shouldn't be a problem for you.: a serious condition that prevents you from engaging in any activity, forces you to skip work or study. In the article we will tell you how to distinguish abnormal uterine bleeding.
How to reach
How to get
From the Belorusskaya metro station of the Zamoskvoretskaya line - exit 4 After exiting the subway, walk through the pedestrian tunnel and climb the stairs. Move towards the railway tracks, go down the stairs immediately after them and walk along the house, then turn right onto 1st Yamskoye Pole Street. At the turn to 3rd Yamsky Pole Street, cross the road at the pedestrian crossing and continue along 1st Yamsky Field Street, after a few buildings on the left you will see Olympus Clinic MARS.
Travel time
9 minutes
Landmark
Olympus Clinic MARS sign
How to get
From the Belorusskaya metro station of the Ring line - exit 2. After exiting the subway, turn left and walk to the pedestrian crossing. Cross the road through two pedestrian crossings and move along the Tverskoy overpass. Go down the stairs immediately after the railway tracks, walk along the house, then turn right onto 1st Yamskoye Pole Street. At the turn to 3rd Yamsky Pole Street, cross the road at the pedestrian crossing and continue along 1st Yamsky Field Street, after a few buildings on the left you will see Olympus Clinic MARS
Travel time
11 minutes
Landmark
Olympus Clinic MARS sign
From the metro station "Tsvetnoy Bulvar"
1 exit to the city, then left to the Garden Ring, at the crossing to the right, crossing the boulevard, one more crossing and at the traffic light to the left. The Olymp Clinic building is located overlooking the Garden Ring to the right of the crossing. Travel time is approximately 9 minutes. Landmark - sign Olymp Clini
From the metro station "Sukharevskaya"
Exit 3 from the metro and 640 meters straight ahead, the clinic will be on the right. Landmark - sign Olymp Clinic
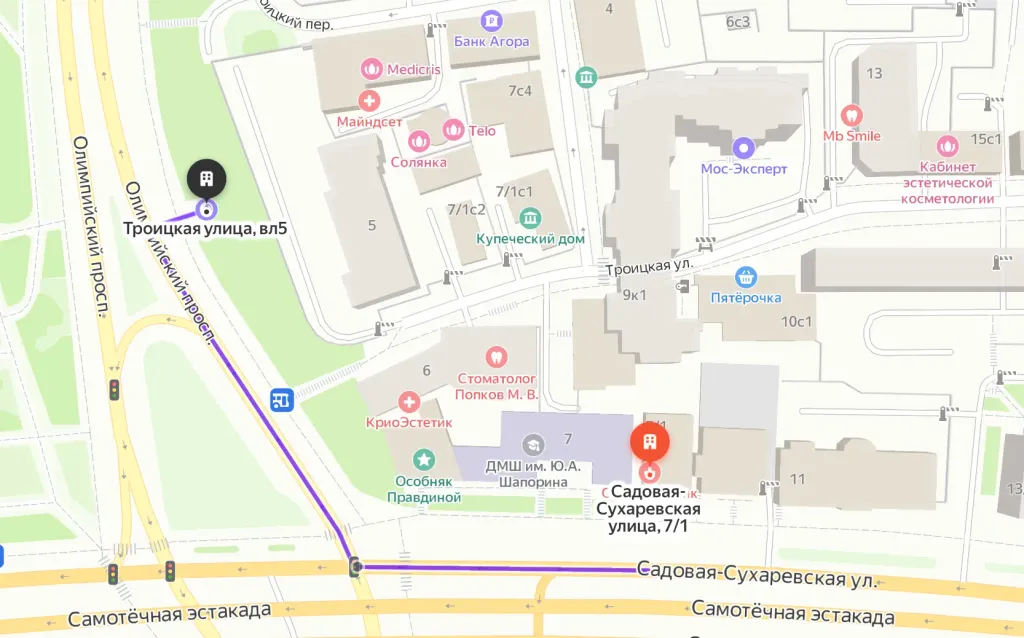
Parking lot map
Exit 3 from the metro and 640 meters straight ahead, the clinic will be on the right. Landmark - sign Olymp Clinic
From Sokol metro station
The last car from the center: follow the signs for Exit 5. From the glass doors to the right and go to the end of the passage. Exit to the city by the steps to the left. After exiting the crossing to the street, go straight along Leningradsky Prospekt to the intersection with Chapaevsky Lane. Next, turn right (onto Chapaevsky Lane) and walk to the Triumph Palace residential complex. Entrance to the territory: through checkpoint No. 1, opposite the Vkusville store, you will need to present your passport. After passing through the checkpoint, go up the stairs to the fountain, opposite it you will see our clinic.
Travel time
10-12 minutes
From the Airport metro station
The first car from the center: follow the Exit 2-3 signs. Turn left out of the glass doors and walk to the end of the passage. After exiting the crossing to the street, go straight along Leningradsky Prospekt to the intersection with Chapaevsky Lane. Next, turn left (onto Chapaevsky Lane) and walk to the Triumph Palace residential complex. Entrance to the territory: through checkpoint No. 1, opposite the Vkusville store, you will need to present your passport. After passing through the checkpoint, go up the stairs to the fountain, opposite it you will see our clinic.
Travel time
12-15 minutes
How to get
Entry to the territory is prohibited, but there are free city parking lots around the Triumph Palace residential complex, where you can easily find a place for your car. Free parking area:

How to get
From the Belorusskaya metro station of the Zamoskvoretskaya line - exit 4 After exiting the subway, walk through the pedestrian tunnel and climb the stairs. Move towards the railway tracks, go down the stairs immediately after them and walk along the house, then turn right onto 1st Yamskoye Pole Street. At the turn to 3rd Yamsky Pole Street, cross the road at the pedestrian crossing and continue along 1st Yamsky Field Street, after a few buildings on the left you will see Olympus Clinic MARS.
Travel time
9 minutes
Landmark
Olympus Clinic MARS sign
How to get
From the Belorusskaya metro station of the Ring line - exit 2. After exiting the subway, turn left and walk to the pedestrian crossing. Cross the road through two pedestrian crossings and move along the Tverskoy overpass. Go down the stairs immediately after the railway tracks, walk along the house, then turn right onto 1st Yamskoye Pole Street. At the turn to 3rd Yamsky Pole Street, cross the road at the pedestrian crossing and continue along 1st Yamsky Field Street, after a few buildings on the left you will see Olympus Clinic MARS
Travel time
11 minutes
Landmark
Olympus Clinic MARS sign








